Stanford PhD student develops novel formula to help donors determine where to put their global aid
As global health assistance for developing countries dwindles, a Stanford student working on her PhD in health policy has developed a novel formula to help donors make more informed decisions about where their dollars should go.
Donors have typically relied predominately on gross national income (GNI) per capita to determine aid allocations. But using GNI is problematic because it effectively penalizes economic growth. It also fails to capture contextual nuances important to channeling aid effectively and efficiently.
So Tara Templin, a first-year Stanford PhD student specializing in health economics, and her Harvard colleague Annie Haakenstad, have developed a framework that estimates funding based on needed resources, expected spending and potential spending into 2030. They believe the more flexible model makes it adaptable for use by governments, donors and policymakers.
“We've observed development assistance for health growth attenuate over the last seven years,” said Templin, who was a research fellow at the Institute for Health Metrics and Evaluation before coming to Stanford. “There are difficult trade-offs, and this entails honing in on the specific challenges and countries most in need.”
Their research published in the journal Health Policy and Planning outlines how their “financing gaps framework” can be adapted to short- or long-run time frames, between or within countries.
“Depending on donor preferences, the framework can be deployed to incentivize local investments in health, ensuring the long-term sustainability of health systems in low- and middle-income countries, while also furnishing international support for progress toward global health goals,” write the authors, who also are Stephen Lim of the University of Washington, Jesse B. Bump of Harvard and Joseph Dieleman, also at the University of Washington.

The authors developed a case study of child health to test out their framework. It shows that priorities vary substantially when using their results as compared to focusing mainly on GNI per capita or child mortality.
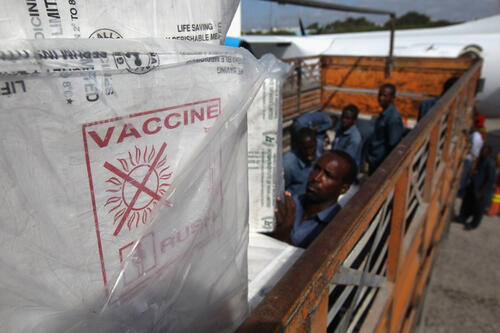
The case study uses data from the Global Burden of Disease 2013 Study, Financing Global Health 2015, the WHO Global Health Observatory and National Health Accounts. Funding flows are anchored to progress toward the U.N. Sustainable Development Goals’ target for reductions in the death rates of children under 5. More than six million children die each year before their fifth birthday, so the United Nations set a goal to reduce under-5 mortality to at least 25 per 1,000 live births.
To build their child health case study, the authors relied on a 2015 study that estimated the average cost per child-life saved is $4,205 in low-income countries, $6,496 in lower-middle income countries and $10,016 in upper-middle countries.
The framework considers three concepts. First, expected government spending is constructed from national health accounts, which are standardized financial reports from countries around the world. Second, ability to pay is estimated by looking at countries with similar levels of economic development and looking at associations with country investment in the health sector. Lastly, needed investment considers a health target, the country’s current health burden, and average costs to save children’s lives in each country.
“Our focus is on the gap between the resources needed to reach critical health targets and domestic health spending,” the authors wrote. “We highlight two facets of domestic health resources—expected spending and potential spending—as critical. While donor preferences may vary, basing aid allocation on expected or existing spending levels incentivizes countries to spend less on health. We therefore propose the use of potential spending, which is a measure of a country’s ability to pay, as the domestic resource benchmark.”
Instead of the gap between expected spending and need, their framework focuses on the gap between potential spending and the health resources needed to meet global health targets. In the framework, policymakers can choose which gap they want to target, since this decision can involve many factors.
“By focusing on that gap, donors can catalyze sustained domestic spending while also addressing the resource needs critical to reaching international health goals,” they wrote.
They then looked at 10 countries with the most need for additional child health resources. The gap between expected spending and potential spending was highest in Afghanistan, at 79 percent, and lowest in Cameroon, where expected spending exceeded potential spending.
“Fifty years ago, GNI was the best proxy for countries’ ability to finance their own development and health,” the authors wrote.
But today, more empirical data and technology are available, allowing donors to incorporate a broader set of health financing measures into their decision-making process.
“The flexible but targeted nature of our framework is critical in the current era of global health financing,” said Haakenstad, the lead author. “Our framework helps to ensure the poor and disadvantaged, the majority of which now reside in middle-income countries, are reached by development assistance and other public financing. This funding is critical to reducing death and disability and reaching global targets in health.”
The authors’ research was supported by the Welcome Trust (099114/Z/12/Z).









 Grace Lee joins Stanford as the Associate Chief Medical Officer at Lucile Packard Children's Hospital in the fall, 2017.
Grace Lee joins Stanford as the Associate Chief Medical Officer at Lucile Packard Children's Hospital in the fall, 2017.

 Rosenkranz Prize 2017 winner Mike Baiocchi and his partner, Clea Sarnquist, both of Stanford Medicine, conduct research on the ground in Nairobi, Kenya, to determine whether a rape prevention program is truly making a difference.
Rosenkranz Prize 2017 winner Mike Baiocchi and his partner, Clea Sarnquist, both of Stanford Medicine, conduct research on the ground in Nairobi, Kenya, to determine whether a rape prevention program is truly making a difference.